
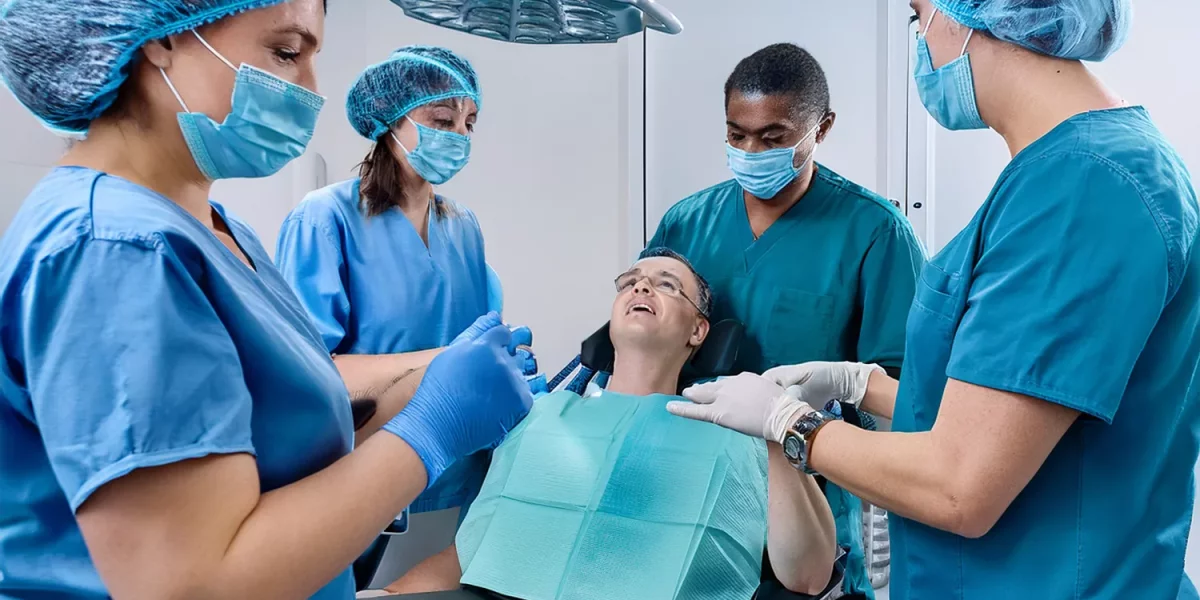
A Practical, Compassionate Approach with Oral and Maxillofacial Surgeon Dr Direnç Ulaşan – Bursa
Providing safe, high-quality dental care to patients with disabilities is one of the most important responsibilities in modern oral and maxillofacial surgery. For many families, simply finding a clinic that truly understands special needs dentistry can feel like a challenge. Questions like…
“Will my child or parent cope in the dental chair?”
“How will they react to the needle and the sounds?”
“Is it safe to do tooth extraction or implant surgery in their condition?”
…are completely normal.
In Bursa, oral and maxillofacial surgeon Dr Direnç Ulaşan focuses on a structured, patient-centred approach to disabled patients – combining medical safety, behavioural understanding and clear communication. This article explains, in detail, how an oral and maxillofacial surgeon can and should approach patients with physical, intellectual, sensory and psychiatric disabilities in a way that is ethical, safe and sustainable, while staying highly relevant for SEO.
“Patients with disabilities” is a broad term. In a real surgical clinic in Bursa, this includes, for example:
Intellectual disabilities
Down syndrome
Global developmental delay
Learning disabilities
Autism spectrum conditions
Sensory sensitivities
Communication differences
Physical disabilities
Cerebral palsy
Neuromuscular disorders
Wheelchair users and mobility limitations
Sensory impairments
Deaf or hard-of-hearing patients
Blind or visually impaired patients
Psychiatric or behavioural conditions
Severe anxiety, phobias and post-traumatic stress
Bipolar disorder, schizophrenia or other complex diagnoses
The key point: each patient is different. A one-size-fits-all approach simply does not work. An oral and maxillofacial surgeon like Dr Direnç Ulaşan in Bursa needs a flexible framework that can be adapted to the needs, communication style and medical status of each person.
The most important instrument in the clinic is not a surgical drill; it is listening.
Before planning any treatment, the surgeon and team should talk to the people who know the patient best:
How does the patient usually react in medical settings?
What are their biggest fears or triggers?
How do they express pain or discomfort – with words, gestures, behaviour changes?
Are there specific sounds, smells or sensations that cause distress?
What has worked well in the past at other clinics or hospitals?
This information allows Dr Direnç Ulaşan to design a personalised pathway – from how long the appointment should be, to whether the patient will need local anaesthesia only, sedation or full general anaesthesia.
For some families, the priority may be:
Stopping chronic pain from decayed teeth
Managing recurring infection around impacted teeth
Preparing the mouth for future medical treatments (for example, before heart surgery or chemotherapy)
In other cases, the focus may be on:
Restoring function so the patient can eat more comfortably
Improving oral hygiene access for caregivers
Managing trauma-related tooth fracture after falls or self-injury
Clarifying these goals helps the surgeon create a realistic treatment plan that balances medical necessity with what the patient can safely tolerate.
A truly special-needs-friendly oral surgery clinic does more than simply install a ramp at the entrance.
Key features include:
Step-free or ramp access for wheelchairs and walkers
Wide doors and corridors for easy turning radius
Accessible toilet facilities
Transfer options for patients who cannot easily move from wheelchair to dental chair
In Bursa, patients and their families should feel that the clinic is physically prepared to welcome them – not that they are an exception.
Many disabled patients, especially those with autism or sensory processing differences, struggle with:
Bright, sharp lights
High-pitched sounds from suction and drills
Strong smells (disinfectants, eugenol, certain dental materials)
Where possible, the team can:
Dim lights or use softer lighting when safe
Allow noise-cancelling headphones or music
Introduce instruments gradually, letting the patient see and even touch them before use
Predictability and control are powerful tools. When patients know what is coming next, they are less likely to panic.
Effective communication is not about using complex medical terms; it is about being understood.
The oral surgeon and team should:
Use short, concrete sentences
Avoid unnecessary jargon
Use simple visual aids or picture cards if needed
Show rather than only tell: “I will spray water now,” while pointing to the device
For deaf or hard-of-hearing patients, written communication, lip-reading support or sign language interpretation may be required. For visually impaired patients, describing each step verbally becomes much more important.
For some patients, especially children with autism, pre-visit desensitisation is very helpful. This might include:
Visiting the clinic before any treatment just to see the room and meet the team
Using “social stories” – simple picture sequences showing the steps of a visit
Practising sitting in the dental chair without any tools in the mouth
An oral and maxillofacial surgeon like Dr Direnç Ulaşan can schedule short, positive visits before any major procedure such as tooth extraction or minor surgery. These “no-pressure” visits build trust and familiarity.
Once trust begins to form, the surgeon can focus on safe diagnosis and planning.
For many disabled patients, a long, detailed examination is impossible. The solution is to:
Break the assessment into manageable parts
Start with the least invasive steps
Use mouth props or support as needed, without forcing
If full examination is not possible in the chair, the surgeon may plan examination under sedation or general anaesthesia, combining diagnostics and treatment in a single, carefully organised session.
Oral and maxillofacial surgeons rely on imaging such as panoramic X-rays and cone beam CT. For some patients, even positioning for an X-ray can be challenging. Skilled teams:
Use additional staff support for safe positioning
Work quickly and calmly
Consider imaging under sedation when absolutely needed
At the same time, medical safety is central:
Reviewing medications and allergies
Understanding seizure risk and triggers
Considering heart, lung or metabolic disease
Discussing anaesthetic risk with physicians for hospital-based procedures
One of the most important clinical decisions for a disabled patient is how to deliver treatment safely.
For some patients, careful local anaesthesia and behavioural support in the dental chair are enough. Success depends on:
A trustful relationship with the surgeon
Clear explanation before the needle is given
Slow, gentle injection technique
Short, efficient treatment sessions
Simple procedures – like small fillings, minor tooth extraction or cleaning – can often be completed under local anaesthesia once the patient accepts the environment.
When local anaesthesia alone is not enough, sedation may be used to:
Reduce anxiety
Decrease movement and muscle tone
Make longer procedures possible
Sedation should always be performed with proper monitoring, emergency protocols and trained staff. An oral and maxillofacial surgeon like Dr Direnç Ulaşan works closely with anaesthesia professionals to choose the safest sedation option for each case.
For patients with severe intellectual disabilities, major behavioural challenges or complex medical conditions, general anaesthesia in a hospital setting can be the most humane option. Under general anaesthesia, the team can:
Perform a full examination
Take all necessary X-rays
Carry out multiple procedures in one session – tooth extractions, restorations, cleaning, minor soft tissue surgery
This “one-session full mouth approach” reduces the number of stressful visits and can stabilise the patient’s oral health for months or years.
In special needs dentistry, prioritisation matters. An oral and maxillofacial surgeon will typically focus on:
Eliminating pain and acute infection
Removing teeth with large abscesses or repeated infections
Treating deep cavities close to the nerve
Managing trauma and tooth fractures
Stabilising or removing severely fractured teeth after falls or accidents
Protecting soft tissues from sharp edges
Creating a mouth that caregivers can clean
Smoothing rough surfaces
Simplifying restorations
Reducing the number of areas that trap food and plaque
Cosmetic priorities come later, once comfort, infection control and safe function are secured.
Successful treatment of disabled patients is a team sport.
Caregivers are not just visitors; they are essential partners. They can help:
Explain the patient’s signals of stress or pain
Assist in positioning or calming the patient
Implement oral hygiene recommendations at home
Monitor healing after surgery and report any concerns early
Written instructions, in clear language, help families feel confident when they leave the clinic in Bursa and return home.
For many disabled patients, the mouth is only one part of a larger health picture. An oral and maxillofacial surgeon may need to coordinate with:
Neurologists (for seizure control and medication interactions)
Cardiologists (for endocarditis risk and anticoagulant management)
Psychiatrists (for behaviour-modifying medications)
Physiotherapists and occupational therapists (for safe positioning and support)
This integrated approach ensures that dental treatment supports – rather than conflicts with – the patient’s overall medical plan.
A single successful treatment under sedation or general anaesthesia is only the beginning. The real challenge is to keep the mouth healthy over time.
Because some patients cannot brush effectively themselves, caregivers need:
Practical training in brushing and interdental cleaning
Advice on toothbrush types, modified handles or electric brushes
Guidance on toothpaste choice, fluoride use and mouthwashes
Short, positive follow-up visits with Dr Direnç Ulaşan can help reinforce habits and monitor vulnerable areas before they become emergencies.
Diet has a huge impact on oral health, especially in patients who may graze on soft, high-sugar foods or use sweetened liquids in bottles or sippy cups for comfort. Discussing realistic diet modifications with families can significantly reduce the risk of new cavities and infections.
While many general dentists provide excellent care, complex disabled patients often benefit from the additional training and hospital access of an oral and maxillofacial surgeon.
With Dr Direnç Ulaşan in Bursa, families gain:
A surgeon trained in both dentistry and facial surgery
Experience in managing difficult extractions, trauma and infections in medically fragile patients
Structured pathways for local anaesthesia, sedation and hospital-based general anaesthesia
A team that understands that behaviour is communication – not misbehaviour
Most importantly, they gain a partner who sees the whole person, not just the teeth.
Patients with disabilities deserve the same level of comfort, safety and respect as any other patient – and often need more planning, not less. A high-quality oral and maxillofacial surgery service in Bursa must therefore offer:
Accessible, sensory-aware facilities
Flexible communication strategies
Skilled use of local anaesthesia, sedation and general anaesthesia
Thoughtful prioritisation of pain relief, infection control and function
Long-term follow-up focused on prevention and caregiver support
The approach of oral and maxillofacial surgeon Dr Direnç Ulaşan is built on a simple principle: no patient is “too difficult” or “too disabled” to deserve proper oral care. With the right team, planning and compassion, even complex surgical needs can be met in a way that protects dignity, reduces fear and gives disabled patients the healthy, comfortable mouths they deserve.
Maximize the lifespan of your implant-supported teeth (crowns, bridges, prostheses). Learn essential long-term maintenance strategies, including correct brushing techniques, specialized flossing tools, and the vital role of regular check-ups for preventing peri-implantitis.
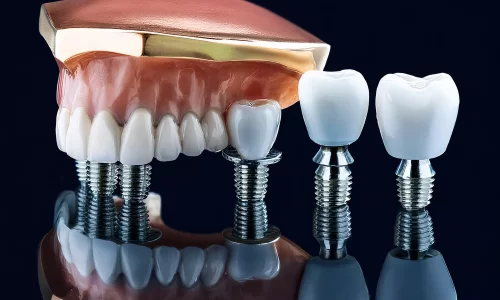
A guide to post-operative care and recovery following zygomatic implant treatment.

Planning dental implants in Turkey? Get a detailed timeline of your treatment, understand the healing process, the duration between stages, and learn exactly what happens regarding aftercare and follow-up once you fly back home.
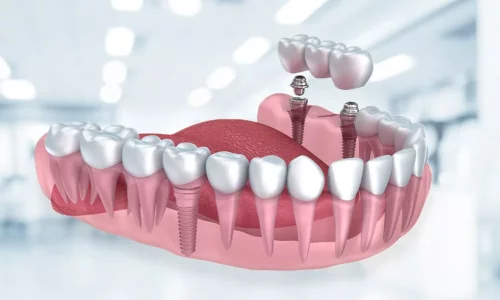
Milim Dental Hospital isn't just a clinic—it's where confident smiles begin. With a team of world-class specialists, advanced technology, and a patient-first approach, we turn dental care into a premium experience.
We prioritize hygiene, comfort, and tailor-made treatments designed just for you. Don’t just take our word for it—explore real stories from real patients.
Your perfect smile starts here. Join the Milim experience.




Milim Dental Hospital provides comprehensive dental services in a spacious 1,000 m² facility, supported by a wide team of dental professionals including specialists in Oral and Maxillofacial Surgery, Prosthodontics, Orthodontics, Pediatric Dentistry, and Periodontology.