
“Will my implant fail?”
“Why didn’t my implant take?”
“What if the implant doesn’t bond with the bone?”
If you’re asking these questions, you’re not alone. Anyone considering a dental implant – or who has already had one placed – worries about the possibility that it might not “take” or might fail later.
The good news:
Modern dental implants have very high success rates when they are:
correctly planned,
placed by an experienced clinician, and
properly maintained by the patient.
But like any medical treatment, implants are not 100% risk-free. Sometimes an implant doesn’t integrate with the bone, becomes loose, or fails after a period of time.
In this article, we’ll answer the question:
“Why might my implant fail?”
We’ll walk through the 10 most common reasons for dental implant failure, what actually happens when an implant “doesn’t take”, and what you can do to reduce your risk and protect your investment.
Patients often say:
“The implant didn’t take.”
“The implant didn’t hold.”
“My implant didn’t fuse with the bone.”
Clinically, what we’re talking about is a problem with osseointegration – the process where the bone grows and bonds tightly to the surface of the implant.
A successful implant should be:
stable (no mobility),
comfortable (no persistent pain),
surrounded by healthy bone and gum tissue, and
able to support normal chewing forces.
If osseointegration doesn’t happen properly, you may see:
a loose implant,
pain when biting,
bone loss around the implant on X-rays,
sometimes the implant even coming out completely.
That’s when people say “my implant failed” or “it didn’t take”.
An implant needs sufficient bone around it to be stable and to withstand chewing forces over time. If the bone is:
too thin,
too short, or
too soft/porous,
the implant may not integrate properly or may become loose later.
Bone loss is especially common when:
a tooth has been missing for many years,
there were old infections in that area,
patients have periodontal (gum) disease,
there are certain systemic conditions or medications affecting bone.
In these cases, you might need bone grafting, sinus lifting or other augmentation procedures before or with implant placement. If bone quantity and quality are not properly evaluated and prepared, it’s one of the most common reasons an implant does not succeed.
Smoking is one of the biggest enemies of dental implants.
Nicotine and other chemicals in cigarettes:
reduce blood flow and oxygen to the tissues,
slow down healing,
increase the risk of infection,
negatively affect bone metabolism.
Studies consistently show that smokers have a higher implant failure rate than non-smokers.
That’s why many surgeons strongly recommend:
stopping smoking before implant surgery,
avoiding cigarettes during the critical healing period,
ideally quitting completely to protect both implants and natural teeth.
Your body doesn’t heal in isolated “compartments”. Your general health directly affects how your mouth heals.
Conditions that can increase the risk of implant failure include:
poorly controlled diabetes,
certain cardiovascular diseases,
disorders or medications that suppress the immune system,
osteoporosis treated with specific medications (e.g. some bisphosphonates).
For example, in uncontrolled diabetes:
wound healing is slower,
infection risk is higher,
bone–implant bonding may be compromised.
A responsible implant clinician will always:
take a thorough medical history,
ask for recent blood tests where appropriate (e.g. HbA1c in diabetics),
coordinate with your physician if needed,
delay or adapt treatment until your condition is better controlled.
Implants are not “install and forget” devices.
They live in a bacterial environment – your mouth.
If plaque and bacteria are not effectively removed, you can develop:
peri-implant mucositis – inflammation of the gum around the implant, and
peri-implantitis – inflammation with bone loss around the implant.
Signs can include:
bleeding when brushing,
bad taste or smell,
tenderness around the implant,
gum recession or exposed implant threads.
If peri-implantitis is not treated in time, it can lead to progressive bone loss and ultimately implant failure.
This is why:
proper brushing technique,
interdental brushes, floss or water flossers,
and regular professional check-ups and cleanings
are absolutely essential for the long-term success of dental implants.
Some implants are placed in areas where there was previously:
an abscessed tooth,
chronic infection, or
a difficult, inflamed extraction.
If:
the infection wasn’t fully resolved,
necrotic or infected bone was left behind,
or an implant was placed too soon in a poorly healed site,
residual infection can re-activate around the implant and prevent proper osseointegration.
A careful surgeon will:
thoroughly clean the extraction site,
sometimes delay implant placement to allow healing,
or combine immediate implants with precise debridement and appropriate medication.
If this stage is rushed or not done meticulously, it can be a hidden reason why an implant later “doesn’t hold”.
Dental implant surgery is not just screwing a metal post into bone. Proper planning and technique are critical.
Common technical or planning-related causes of failure include:
placing the implant at the wrong angle or depth,
insufficient primary stability at surgery,
overheating the bone during drilling,
putting implants too close together or too close to neighbouring teeth,
ignoring anatomical structures (sinus, nerve, etc.).
These issues can:
compromise blood supply,
create excessive stress on the implant,
or make it impossible to design a proper, cleanable crown or bridge.
Today, many clinicians use 3D imaging (CBCT) and digital or guided surgery to improve accuracy and reduce such risks. Choosing an experienced implant surgeon with a strong planning protocol significantly lowers the chance of failure from technical errors.
Even a perfectly placed implant needs time to integrate with the bone. Depending on the case, this can be weeks to several months.
Problems arise when:
an implant is loaded too early (you chew hard before the bone has bonded),
the bite is not properly adjusted and one implant takes too much force,
chewing habits put excessive load on the implant and crown.
This is called overloading, and it can:
disturb the healing process,
cause micro-movements in the bone–implant interface,
eventually lead to loss of osseointegration.
In some cases, immediate loading (placing a temporary tooth on the implant right away) is safe — but only when the surgeon is confident that:
primary stability is high,
the bite is carefully controlled,
and the patient understands the limitations on chewing.
Your jaw muscles are powerful. If you clench or grind your teeth, especially at night, you create excessive forces on teeth and implants.
These forces can:
cause micro-fractures in the bone,
loosen screws or abutments,
chip or break crowns,
and, over time, contribute to implant failure.
Other sources of overload include:
hitting the jaw in an accident or sports injury,
biting hard objects (ice, pens, very hard nuts, etc.),
asymmetrical chewing only on one side.
If you know or suspect that you grind your teeth, tell your dentist. Often, a night guard or adjustments to your bite can protect your implants and your natural teeth.
Your implant surgeon will give you a detailed list of do’s and don’ts after surgery. These instructions are not optional – they are part of the treatment.
Common post-op mistakes that can increase failure risk:
Chewing on the implant side too soon,
Smoking heavily right after surgery,
Vigorous rinsing and spitting in the first 24 hours,
Touching or playing with the surgical area with fingers or tongue,
Not taking prescribed medications as directed,
Skipping follow-up appointments.
Think of the implant site as a delicate construction zone. The body needs time and stability to build the bone–implant connection. Anything that disturbs the clot, increases bacteria, or stresses the area too early can jeopardize osseointegration.
Not all implants and restorations are created equal.
Factors on the “hardware” side that can influence outcomes:
use of low-quality or unproven implant systems with little scientific data,
poorly fitting abutments and crowns,
cheap materials with inferior mechanical properties,
rushed or low-quality laboratory work.
These can lead to:
micro-gaps and bacterial leakage,
screw loosening,
crown fractures,
chronic irritation and inflammation around the implant.
High-quality implants and prosthetic components, combined with a good lab and meticulous fitting by your dentist, are a key part of long-term success.
Not necessarily.
If an implant hasn’t integrated or has become loose, the usual steps are:
Clinical and radiographic assessment – how much bone is lost, what the soft tissues look like, what symptoms you have.
If the implant is mobile, it is typically removed in a controlled way.
The site is cleaned thoroughly; in many cases, a bone graft is placed to rebuild the area.
A healing period follows, during which your health, habits and risk factors are reassessed.
Once the area is stable and the original reason for failure is addressed (smoking, uncontrolled diabetes, overload, etc.), a new implant may be placed with a revised plan.
In other words:
A failed implant does not always mean you can never have an implant again.
What matters is understanding why it failed and preventing the same problem next time.
You can’t control everything, but you can significantly improve your odds by focusing on what is in your hands:
Choose an experienced clinician, ideally with strong surgical and restorative training in implantology.
Be completely honest about your medical history, medications and habits.
If you smoke, quit or reduce as much as possible before and after surgery.
Work with your physician to keep conditions like diabetes well controlled.
Follow all post-operative instructions exactly.
Maintain excellent daily oral hygiene (brushing, interdental cleaning).
Keep all scheduled follow-up appointments – even if you “feel fine”.
Protect your implants with a night guard if you grind or clench.
Avoid biting very hard objects with your implant crowns.
Implants are one of the best investments you can make in your oral health – but like any investment, they need protection and maintenance.
Contact your dentist or implant surgeon as soon as possible if you notice:
mobility (the implant/implant tooth feels loose),
pain when biting that doesn’t get better,
persistent swelling, redness or warmth around the implant,
pus or any discharge from the gum around the implant,
gum recession exposing part of the implant,
sudden changes in your bite or in how your teeth meet.
Early diagnosis and treatment can often save an implant or at least stop the problem from getting worse.
Asking “Why might my implant fail?” is not being negative – it’s being responsible.
It pushes you to:
choose your surgeon carefully,
take your general health seriously,
commit to good oral hygiene and regular check-ups,
see your implant as a long-term partnership between you and your dental team.
When:
the right patient,
the right plan,
the right surgeon, and
the right maintenance
come together, dental implants can function comfortably and beautifully for many years.
If you already have implants or you’re planning to get them, use this information as a checklist. Discuss your risk factors openly with your dentist or oral and maxillofacial surgeon, ask questions, and don’t be afraid to seek a second opinion for complex cases.
Knowledge doesn’t increase fear – it builds confidence. And confidence is exactly what you deserve when you’re making a long-term decision about your smile.
Are all clear aligners the same as Invisalign? Bursa Orthodontic Specialist Dr. Begüm Ulaşan explains the critical differences in material, software, and predictability between brands. Learn what 'Invisalign Provider' means and why the doctor is more important than the brand.
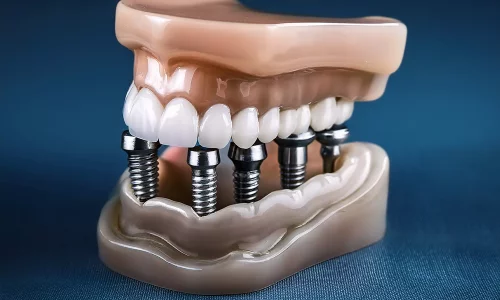
If I get implants, will my teeth be fixed (non-removable)? Compare fixed solutions (crowns, bridges) against removable implant-supported dentures and discover which permanent, functional dental implant restoration is best suited for your needs.
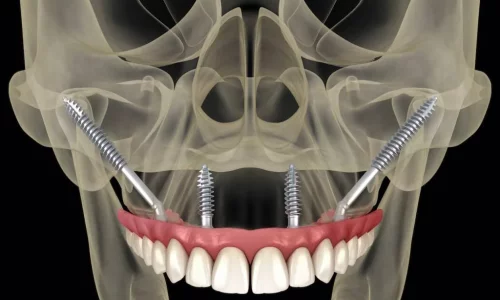
Dental implants have revolutionized the field of restorative dentistry by providing patients with a long-lasting and natural-looking solution to missing teeth. However, for patients with significant bone loss in the upper jaw, traditional implants may not be an option without undergoing bone grafting procedures.
Milim Dental Hospital isn't just a clinic—it's where confident smiles begin. With a team of world-class specialists, advanced technology, and a patient-first approach, we turn dental care into a premium experience.
We prioritize hygiene, comfort, and tailor-made treatments designed just for you. Don’t just take our word for it—explore real stories from real patients.
Your perfect smile starts here. Join the Milim experience.




Milim Dental Hospital provides comprehensive dental services in a spacious 1,000 m² facility, supported by a wide team of dental professionals including specialists in Oral and Maxillofacial Surgery, Prosthodontics, Orthodontics, Pediatric Dentistry, and Periodontology.